There is something quietly reassuring about getting answers sooner instead of later. Not perfect answers in five minutes, not dramatic promises, just a clearer idea of what is happening and what should come next. In 2026, that is one of the biggest reasons more people are paying attention to how medical imaging fits into everyday care.
For a lot of patients, the hardest part is not even the test itself. It is the waiting, the uncertainty, and that awkward in-between stage where something feels off but nothing has been confirmed yet. Maybe there is lingering pain that has not gone away. Maybe a provider noticed something during a routine exam. Maybe symptoms are vague, inconsistent, or frustratingly hard to explain. In situations like that, imaging can help move the conversation forward.
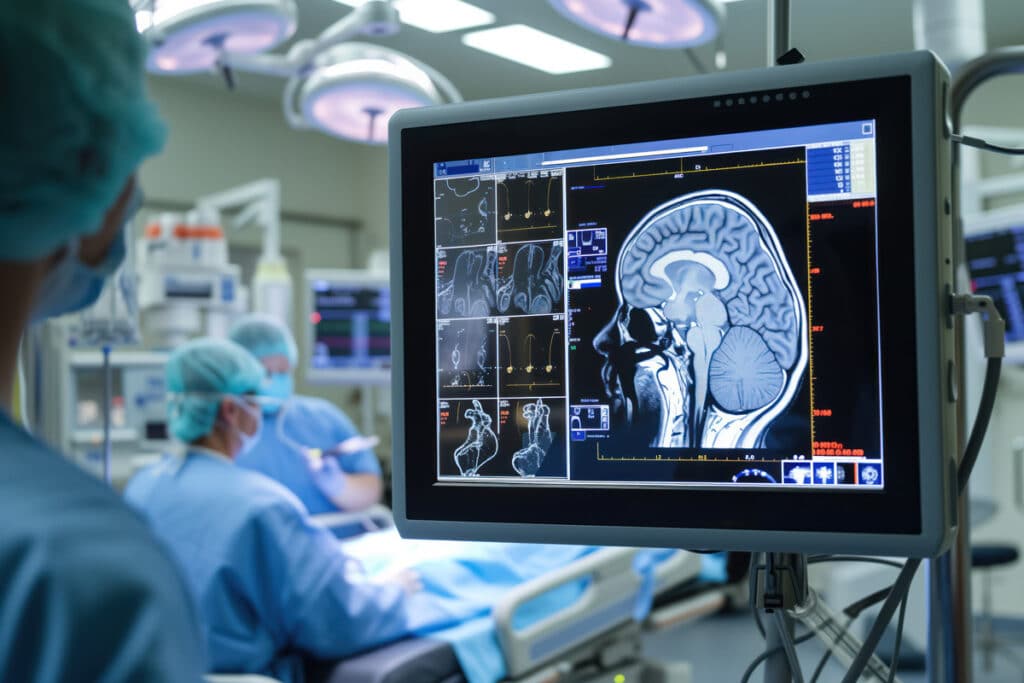
That is where a diagnostic imaging center becomes incredibly valuable. It gives providers a way to look deeper, gather useful information, and avoid making decisions based only on guesswork. And for patients, that can mean less spiraling, fewer assumptions, and a faster path toward understanding what is actually going on.
Why faster answers matter more than ever
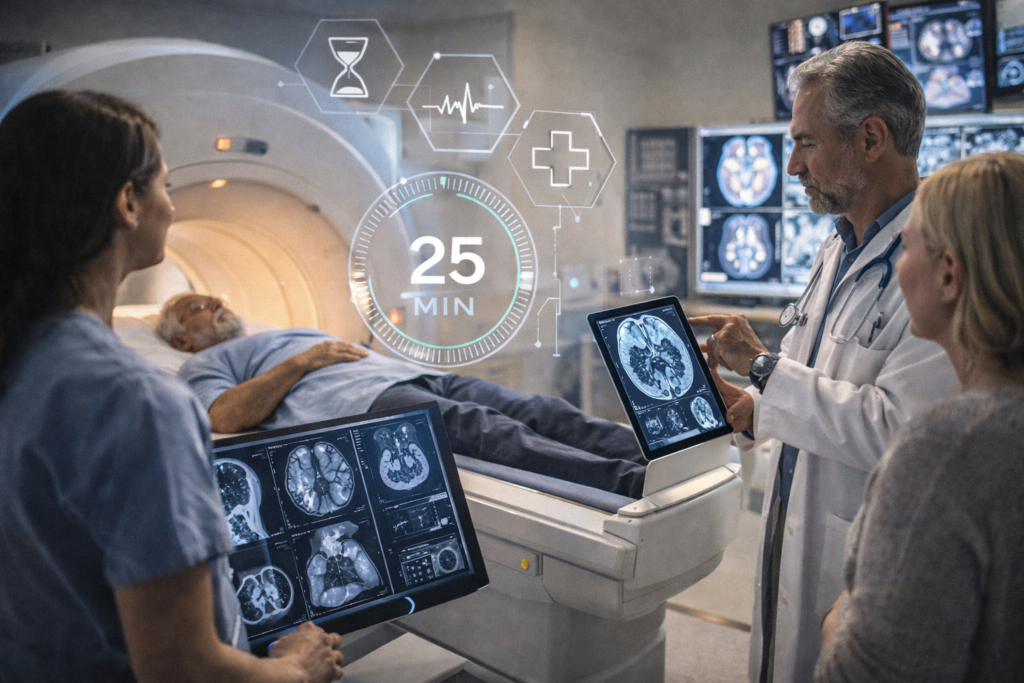
People are more proactive about their health than they were a few years ago. They ask more questions. They pay closer attention to changes in their body. They also tend to notice when something feels delayed or unclear. In that context, faster answers are not just convenient. They can reduce stress and help patients feel like they are doing something productive instead of just waiting around for the next phone call.
That does not mean imaging replaces clinical judgment. It means it supports it. When a provider has a clearer picture of what may be happening internally, the next step often becomes easier to define. That could mean more confidence in a treatment plan, a decision to monitor something over time, or the need for a more focused evaluation.
The point is simple: answers lead to action, and action usually feels better than uncertainty.
The shift toward early detection
One of the biggest healthcare conversations in 2026 centers around early detection. And honestly, it makes sense. Most people would rather learn about a concern at an earlier stage, when there is more time to understand it, manage it, and discuss options calmly. Waiting until symptoms become severe is rarely anyone’s ideal plan.
This is especially true because many health issues do not announce themselves loudly at first. Some begin with small changes that are easy to dismiss. Others cause vague symptoms that overlap with a dozen less serious explanations. A person might assume the issue is stress, fatigue, aging, or just a temporary discomfort. Sometimes that is true. Sometimes it is not.
Imaging helps narrow the field. It offers a closer look when symptoms, physical findings, or lab results suggest that more information is needed. That does not mean every scan reveals something serious. In fact, many provide reassurance. But reassurance backed by real information tends to feel much more solid than reassurance based on hope alone.
How imaging helps reduce uncertainty
There is a big difference between “we think” and “we can see.” That difference matters when patients are anxious, providers are trying to make smart decisions, and timing is important.
At a practical level, imaging can help:
- clarify whether a finding looks benign or needs more attention
- show the size, shape, or location of an abnormal area
- provide more context when symptoms are hard to interpret
- support follow-up planning instead of vague watch-and-wait advice
- help patients feel like the process is moving forward
That last part matters more than people sometimes realize. Feeling stuck in medical uncertainty can be exhausting. Even when the answer is not immediate, a clear next step can be a huge relief.
This is also why patients often appreciate care that feels organized and thoughtful. They want the experience to feel efficient, but they also want it to make sense. Good communication around imaging can make a real difference in how supported a person feels during a stressful moment.
Supporting providers and patients at the same time
A lot of the value of imaging happens behind the scenes. Patients may see the appointment as one more step in a longer healthcare process, but for providers, the information from that exam can shape what happens next in very concrete ways.
Sometimes the question is broad: what could be causing these symptoms? Other times it is much more focused: does this area need additional workup, or can it be monitored? Either way, a radiology center in El Paso can help connect the dots between concern and clarity.
That support matters in everyday cases as much as in more complex ones. Not every patient walks in with a dramatic symptom story. Some just have subtle changes that need context. Others are following up on something that appeared during a routine visit. And many simply want to stop wondering.
In all of those situations, imaging becomes part of a bigger care conversation. It is not just about producing images. It is about producing useful direction.
When serious concerns need clearer answers
Of course, one reason this topic gets so much attention is that imaging can play a role in identifying conditions that require timely care. That includes situations where providers are considering cancer diagnosis as part of the differential. Nobody loves hearing that phrase, even as a possibility. But having the right tools to evaluate concerns early can make a difficult situation feel less chaotic and more manageable.
The same goes for tumor detection, which often depends on getting a detailed look at an area that raised concern during an exam, screening, or previous report. Patients do not need dramatic language in those moments. They need clear information, calm guidance, and a process that feels steady instead of overwhelming.
Imaging can help provide that sense of structure. It does not answer every question all at once, but it often gives enough direction to define what should happen next. And sometimes, that next step is exactly what a patient has been waiting for.
It is not always about major disease
One of the most useful things about modern imaging is that it does not only help in worst-case scenarios. Plenty of scans are ordered for issues that may turn out to be manageable, temporary, or less serious than the patient feared. That matters too.
Take inflammation, for example. It can show up in different parts of the body and for many different reasons. Sometimes it is linked to injury, irritation, chronic conditions, or an active process that needs a closer look. Without imaging, those symptoms can remain frustratingly vague. With imaging, providers often have a better starting point for understanding what the body is responding to and how to manage it.
That is one reason patients should not assume imaging automatically means bad news. Often, it simply means someone wants a more complete picture before making recommendations. That is not alarming. It is responsible.
What patients want from the process in 2026
By now, most people expect healthcare to be more human. They want straightforward explanations, less intimidating experiences, and a process that does not leave them feeling lost. That expectation absolutely applies to imaging.
Patients tend to value a few things the most:
- appointments that feel organized and efficient
- instructions that are easy to understand
- communication that sounds natural instead of overly technical
- a team that understands uncertainty can be stressful
- follow-up that feels connected to the bigger picture of care
This is where experience and tone matter. A calm, conversational approach helps patients feel seen as people, not just as scheduled exams. And when a medical visit feels more human, people are usually better able to move through it with less anxiety.
Final Thoughts
Getting answers sooner can change the entire tone of a healthcare journey. It reduces the mental weight of not knowing, helps providers make more informed decisions, and gives patients a clearer sense of direction when uncertainty starts to take over. In 2026, that kind of clarity matters more than ever. People want care that feels responsive, grounded, and easier to navigate, especially when their health is involved. And when the process helps replace guessing with understanding, even one appointment can make a meaningful difference.