For a long time, people tended to think about imaging as something you only needed after a problem showed up. You felt pain, noticed a symptom, got referred, and then came the test. That mindset is changing. In 2026, more patients are starting to see imaging as part of staying ahead of potential health issues, not just reacting to them.
At Professional Radiology El Paso, that shift feels especially relevant right now. Preventive care is becoming more personal, more proactive, and a lot more practical than it used to be. People are asking better questions. They want to understand what’s happening inside their bodies before a small concern becomes a bigger one. They are also more open to routine screening and follow-up exams that can offer peace of mind or help catch something early.
That change matters because preventive imaging is not about fear. It is about clarity. It is about using the right tools at the right time so patients and providers can make smarter decisions without unnecessary delays. And in a busy city where people are juggling work, family, appointments, and everyday stress, that kind of clarity can make a real difference.
Preventive imaging is becoming part of everyday health
One of the biggest changes in 2026 is that people no longer see advanced imaging as something distant or intimidating. It is becoming part of regular health conversations. Instead of waiting until symptoms become impossible to ignore, patients are being more intentional about screenings, follow-ups, and physician-recommended exams.
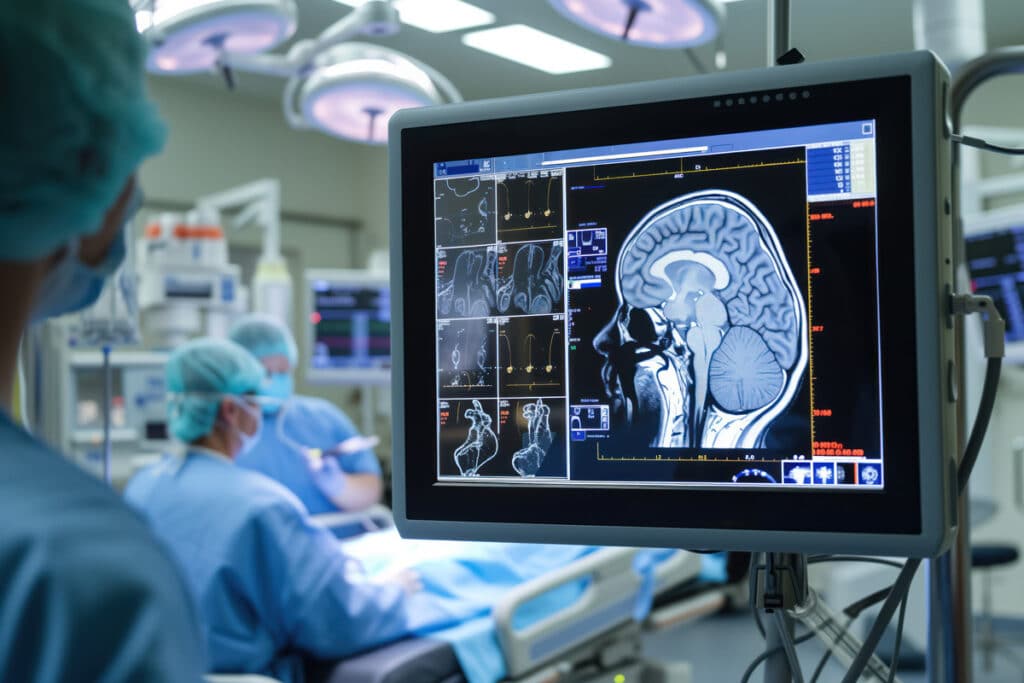
This new era includes a wider understanding of what imaging can do. Some tests are designed to look closely at bones, organs, or soft tissue. Others support screening efforts or help providers take the next step when something needs a closer look. Together, they create a more complete picture of a person’s health.
Preventive imaging may be recommended for many reasons, including:
- routine screenings based on age or family history
- follow-up after an abnormal exam or lab result
- evaluation of a lump, swelling, or unexplained discomfort
- closer review of areas that need more detail
- support for earlier, more informed treatment decisions
What makes this moment different is that patients are more engaged in the process. They are not just showing up because someone told them to. They want to know why a test matters, what it looks for, and how it can help them stay one step ahead.
Screening is no longer something to postpone
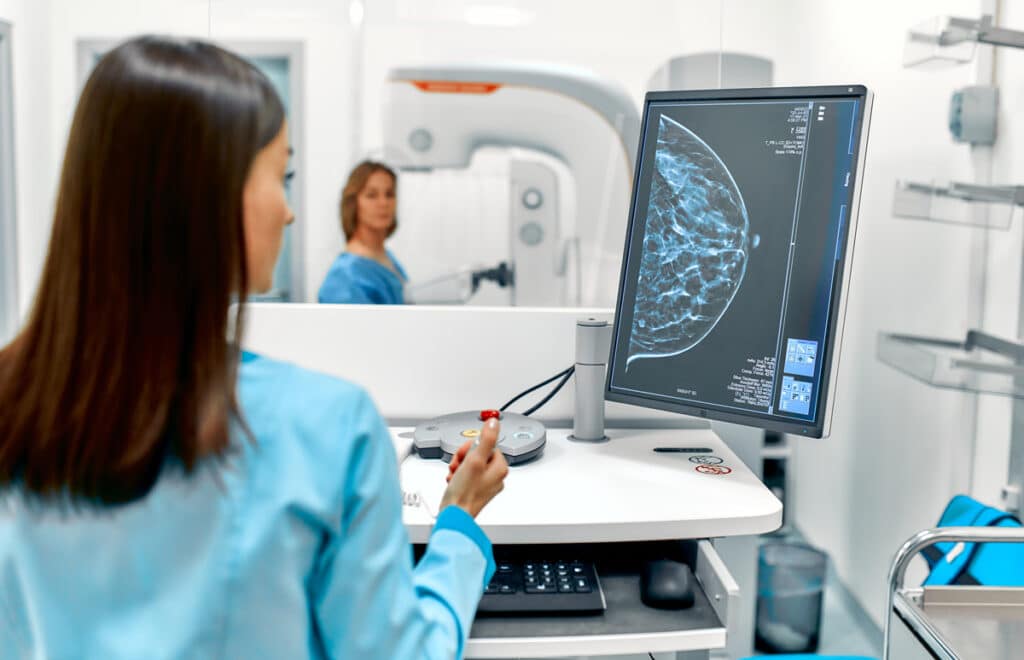
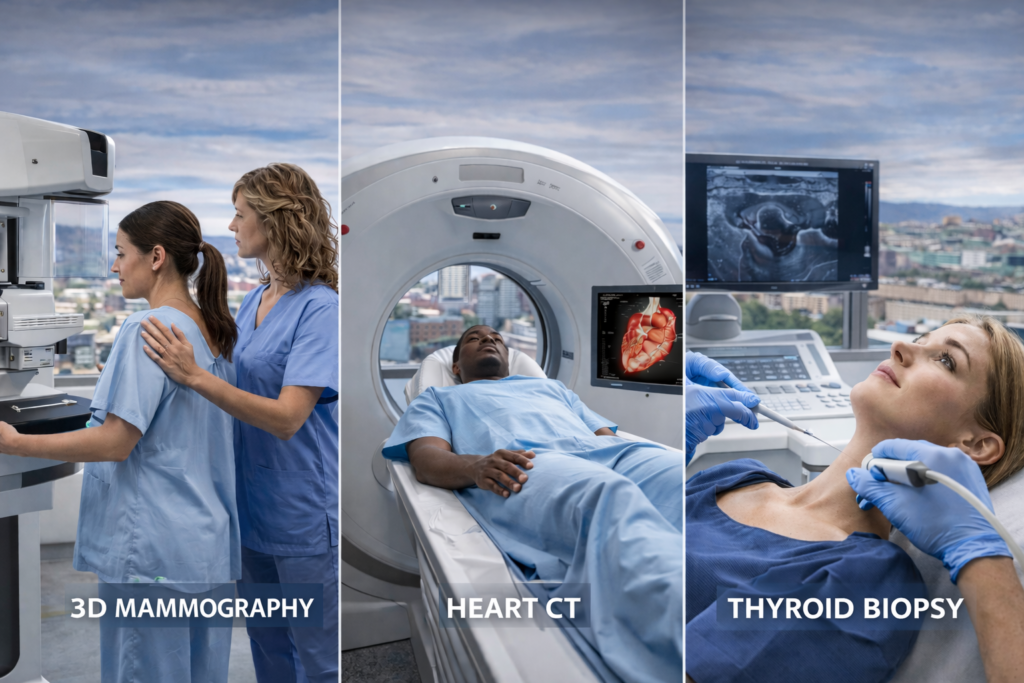
For many women, preventive care often starts with mammography. It remains one of the most important tools in routine screening because it can identify changes that may not be noticeable during daily life. That matters because early awareness often opens the door to more options and less uncertainty.
In 2026, more patients are also hearing about 3D mammography as part of a modern approach to screening. The reason it gets so much attention is simple: people want imaging that feels more precise and more useful, especially when they are trying to make confident decisions about what comes next. Preventive care works best when the process feels clear instead of overwhelming.
At the same time, conversations around breast imaging are becoming more informed. Patients are realizing that screening is not always one-size-fits-all. Depending on a person’s history, symptoms, or prior results, providers may recommend a closer evaluation to better understand what is going on. That can help reduce guesswork and move the process forward in a calmer, more informed way.
Looking beyond one type of exam
Preventive imaging is broader than many people realize. While screenings get a lot of attention, there are several other tools that can help evaluate concerns before they escalate or provide answers when something needs follow-up.
For example, ultrasound is often part of the conversation when providers want a real-time look at soft tissues or specific areas of concern. Patients usually appreciate that it feels familiar, accessible, and easy to understand. It is one of those exams that tends to make preventive care feel less intimidating because the process is often straightforward.
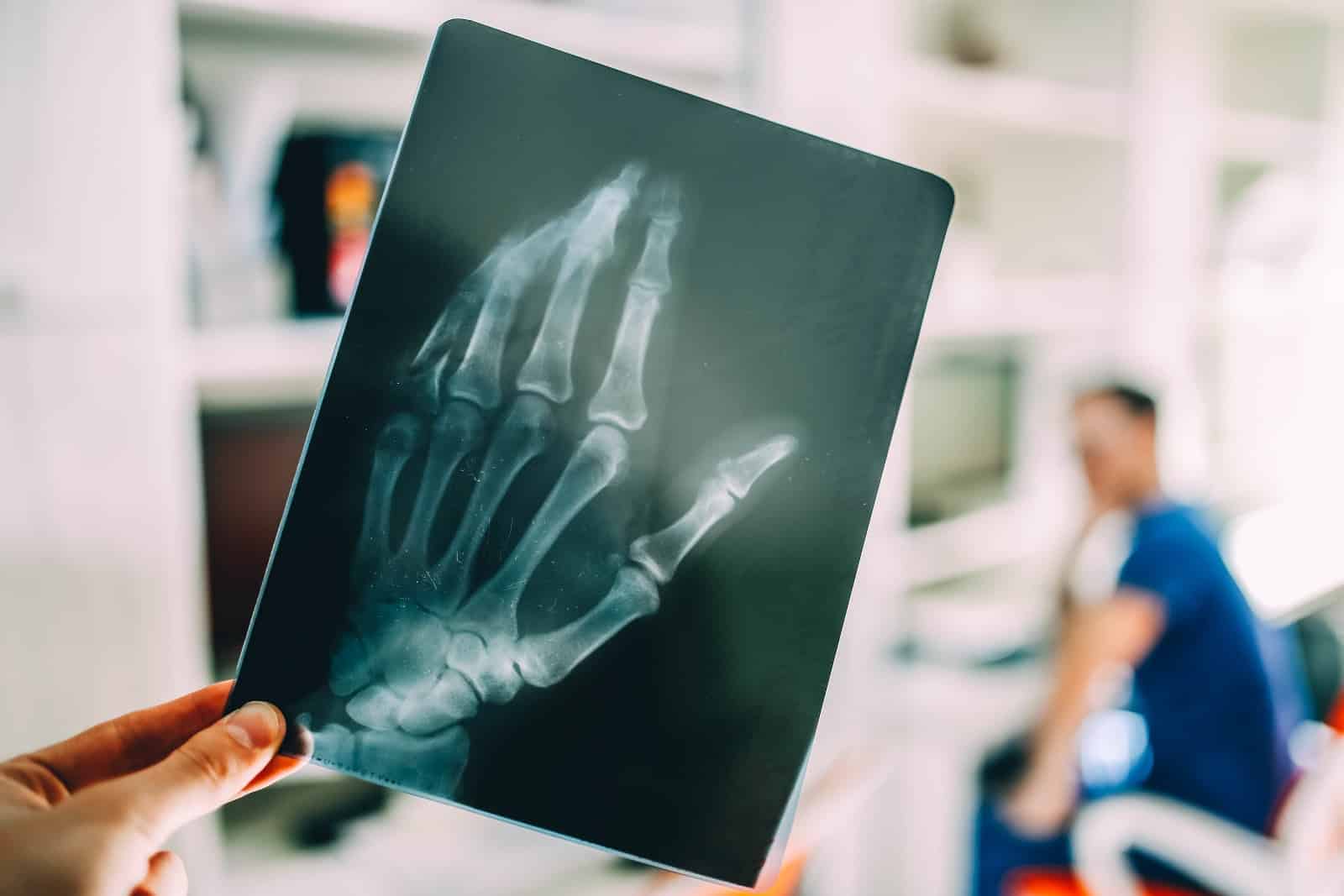
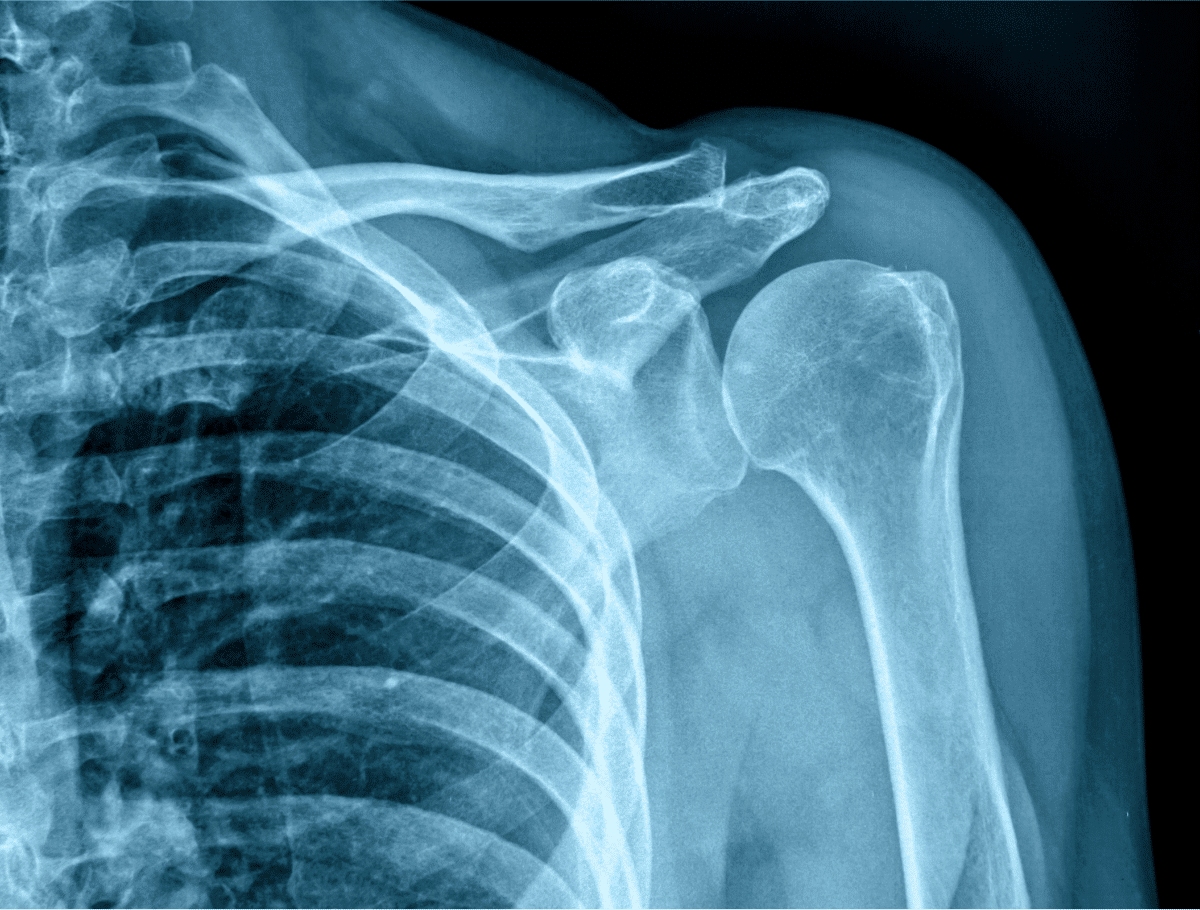
In other situations, digital X-ray may be used when a quick image is needed to assess structure and support a provider’s next steps. Even though it sounds simple compared with newer technologies, it still plays an important role in the bigger picture of timely evaluation and decision-making.
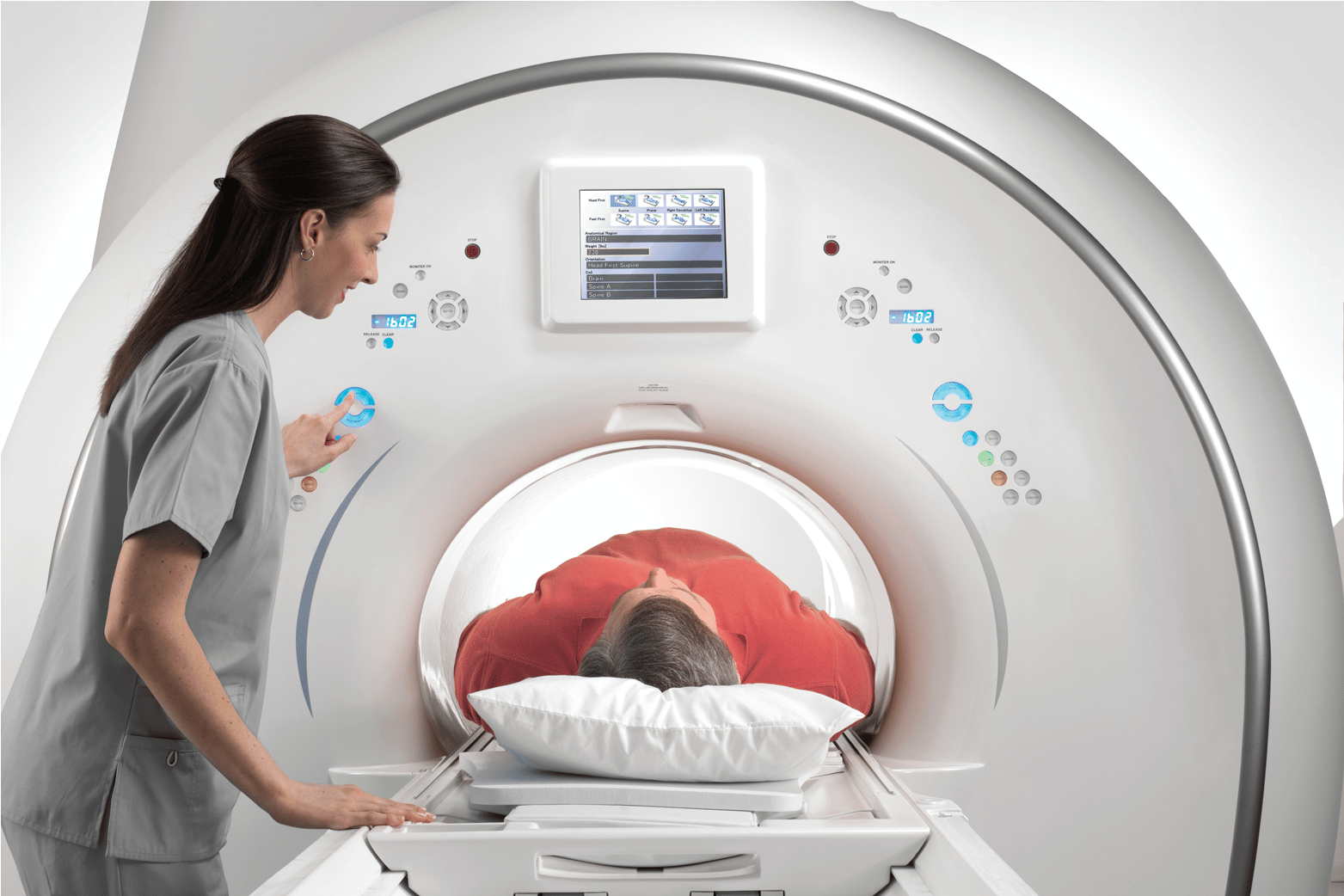
Then there are CT scans, which continue to be valuable when a more detailed internal view is needed. Patients often hear the formal term computed tomography scans during referrals or medical discussions, but what matters most is understanding why a provider chose that option. Preventive care becomes much easier to follow when people understand the purpose behind the exam instead of just hearing a technical name.
When follow-up matters just as much as screening
Not every preventive imaging visit begins with a routine screening. Sometimes it starts with a conversation about something unexpected. A patient notices a lump. A provider feels a nodule during an exam. A report suggests that an area deserves a closer look. This is where imaging often moves from broad screening into more targeted evaluation.
That next step may include biopsies, which can sound intimidating at first simply because the word carries a lot of emotional weight. But in reality, these procedures are often part of getting clearer answers, especially when a provider wants to understand a finding instead of making assumptions.
In some cases, fluid removal or sampling may involve aspirations, depending on what is being evaluated. These are the kinds of details patients rarely talk about until they need them, yet they are central to how preventive medicine actually works. Catch something, evaluate it carefully, and keep moving toward a clearer answer.
A more specific example is fine-needle aspiration, which is often recommended when a provider needs a minimally invasive way to sample cells from a suspicious area. It is one of those procedures that sounds more overwhelming than it usually is. Once patients understand the purpose, the process tends to feel much more manageable.
Thyroid and breast concerns deserve timely answers
Preventive imaging also matters because some concerns are easy to ignore at first. A small neck lump may not feel urgent. A change in breast tissue may seem subtle. Life gets busy, and many people tell themselves they will deal with it later. But later is not always the best plan.
When the thyroid needs a closer look, a provider may recommend a thyroid biopsy to better understand whether a nodule or abnormality requires further care. Having that option available can help patients move from uncertainty to information, which is often the hardest part of the process.
The same is true when a more focused exam leads to a breast biopsy. That step can feel emotionally heavy, but it also provides direction. Instead of sitting with unanswered questions, patients get a clearer path forward. And honestly, that is a huge part of what modern preventive care is all about.
Why this matters in El Paso right now
The new era of preventive imaging is not really about technology alone. It is about access, awareness, and timing. People are becoming more proactive because they understand that waiting does not make uncertainty easier. It usually just makes it longer.
That is why preventive imaging continues to gain momentum:
- it supports earlier conversations about health
- it helps clarify findings before they become bigger concerns
- it gives providers more information for personalized decisions
- it encourages patients to stay engaged in follow-up care
- it makes the path from screening to next steps more organized
In a community like El Paso, that practical approach matters. People want care that feels efficient, understandable, and grounded in real life. They are not looking for complicated language or dramatic messaging. They want straightforward answers, thoughtful guidance, and a process that respects their time and concerns.
Final Thoughts
Preventive imaging is becoming less about reacting late and more about paying attention sooner. That shift is making healthcare feel more proactive, more personal, and ultimately more useful for everyday patients. When people understand their options and feel supported through the process, they are much more likely to stay engaged in their care. And that may be the most important change of all in 2026: people are not just waiting for answers anymore. They are actively choosing to look for them earlier.